Translations may contain older or less detailed information than the original German page!
Normal Mast cell function in Healthy People
Page overview:
Summary:
Discovery and naming
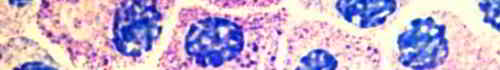
Mast cells (also called mastocytes) were named so by their discoverer because under the microscope they look as if they had been fed up or fattened. This is called "mast" in agriculture (in German: Mast). However, the numerous small granules inside the cell are not nutrients. They serve to store messenger substances (chemical signalling substances) and to release them in certain situations.
Origin and occurrence of mast cells

The mast cells originate in the bone marrow from dividing precursor cells (stem cells). They migrate through the body into the organs in order to fulfil their task there. The mast cells are mainly found in boundary organs and tissues, where there is contact with the hostile outside world (intestinal mucosa, respiratory tract, skin), as well as in the vicinity of vessels and nerves.
Structure and normal function of mast cells
Mast cells are part of the immune system. As "guards" they are responsible for the recognition of parasites, allergens and foreign matter. If necessary, they alert the surrounding tissue by releasing histamine and around 200 other messenger substances. The recognition of "foreign" substances is carried out via various receptors on the mast cell surface, which - similar to sensors - recognise certain chemical structures and on contact can transmit a biochemical signal into the interior of the mast cell. Important examples are the FcεRI receptors as antibody docking sites (allergen contact triggers allergic reactions) and the histamine receptors (histamine activates the mast cell via the histamine H1 receptor, which in turn releases histamine).
Activation and mediator release
The release of mediators is not an uncontrolled bursting of the cell. Depending on the situation only certain mediators can be selectively released, suddenly or continuously. The sudden decay of the mast cell is called degranulation or mast cell degranulation.
In addition to antigen-antibody-mediated immune reactions, there are also numerous substances and other stimuli that lead to unspecific mast cell activation ("pseudoallergies").
The most important mediators (messengers) causing symptoms are histamine, prostaglandin D2 (PGD2), platelet activating factor (PAF), proinflammatory cytokines, LTC4 and LTD4, chemokines and tryptase. Depending on the type, quantity and location of the release, the individual messenger substances have various tasks in the fight against intruders, e.g. inflammatory reactions, mucus secretion, vascular permeability, bronchoconstriction, bowel emptying, ...
The released mediators first reach only the spaces between the cells, where lymph fluid circulates, and are thus distributed in the tissue. There they bind to their specific receptors on the surfaces of the surrounding cells. Once released, the mediators are rapidly degraded before they can enter the lymphatic system or bloodstream. Only when the amount released has increased so much that the local binding and degradation capacity is exhausted can mediators enter the blood. This makes diagnosis more difficult because the mediators can already cause complaints in individual organs without being detectable in the blood.
Guided tour: Go to page
Disease > Pathomechanism
References and bibliography
The "back"-button of your browser takes you back to the previous position.
| G | Back to the previous position |
|---|---|
| Gao et al. 2012 | Gao ZG, Wei Q, Jayasekara MP, Jacobson KA.: "The role of P2Y(14) and other P2Y receptors in degranulation of human LAD2 mast cells.". Purinergic Signal. 2012 Jul 24. http://www.ncbi.nlm.nih.gov/pubmed/22825617 |
| Gao et al. 2010 | Gao ZG, Ding Y, Jacobson KA.: "P2Y(13) receptor is responsible for ADP-mediated degranulation in RBL-2H3 rat mast cells.". Pharmacol Res. 2010 Dec;62(6):500-5. Epub 2010 Sep 8. http://www.ncbi.nlm.nih.gov/pubmed/20813187 |
| M | Back to the previous position |
| Mastcellmaster | T.C. Theoharides. "Molecular Immunopharmacology and Drug discovery Laboratory". http://mastcellmaster.com/research.html (12.06.2012) |
| Molderings 2010 | Molderings GJ.: "Mast cell function in physiology and pathophysiology." BIOTREND Reviews 2010; 5: 1–9. https://www.biotrend.com/download/BTReview_Jan2010_Mastcell.pdf |
| O | Back to the previous position |
| Orfanos 1966 | C. Orfanos: "Mastzelle und Mastzelldegranulation". Klinische Wochenschrift, 15. Oktober 1966, Volume 44, Issue 20, pp 1177-1182. http://link.springer.com/article/10.1007%2FBF01742094 |
| S | Back to the previous position |
| Sudo et al. 1996 | Sudo N, Tanaka K, Koga Y, Okumura Y, Kubo C, Nomoto K.: "Extracellular ATP activates mast cells via a mechanism that is different from the activation induced by the cross-linking of Fc receptors". J Immunol. 1996 May 15;156(10):3970-9. http://www.ncbi.nlm.nih.gov/pubmed/8621938 |
| V | Back to the previous position |
| Valent et al. 2012 | Valent P, Akin C, Arock M, Brockow K, Butterfield JH, Carter MC, Castells M, Escribano L, Hartmann K, Lieberman P, Nedoszytko B, Orfao A, Schwartz LB, Sotlar K, Sperr WR, Triggiani M, Valenta R, Horny HP, Metcalfe DD.: "Definitions, criteria and global classification of mast cell disorders with special reference to mast cell activation syndromes: a consensus proposal". Int Arch Allergy Immunol. 2012;157(3):215-25. Epub 2011 Oct 27. http://www.ncbi.nlm.nih.gov/pubmed/22041891 (Propose a global unifying classification of all MC disorders and pathologic MC reactions. This classification includes three types of 'MCA syndromes' (MCASs), namely primary MCAS, secondary MCAS and idiopathic MCAS. MCA is now defined by robust and generally applicable criteria, including (1) typical clinical symptoms, (2) a substantial transient increase in serum total tryptase level or an increase in other MC-derived mediators, such as histamine or prostaglandin D(2), or their urinary metabolites, and (3) a response of clinical symptoms to agents that attenuate the production or activities of MC mediators.) |
| W | Back to the previous position |
| Wu 2015 | Wu H, Zeng M, Cho EY, Jiang W, Sha O: "The Origin, Expression, Function and Future Research Focus of a G Protein-coupled Receptor, Mas-related Gene X2 (MrgX2)." Prog Histochem Cytochem. 2015 Jun 8. pii: S0079-6336(15)00014-5. doi: 10.1016/j.proghi.2015.06.001. http://www.ncbi.nlm.nih.gov/pubmed/26106044 |
| Y | Back to the previous position |
| Yip et al. 2014 | Yip KH, Kolesnikoff N, Yu C, Hauschild N, Taing H, Biggs L, Goltzman D, Gregory PA, Anderson PH, Samuel MS, Galli SJ, Lopez AF, Grimbaldes-ton MA: "Mechanisms of vitamin D3 metabolite repression of IgE-depen-dent mast cell activation." J Allergy Clin Immunol. 2014 May;133(5):1356-64, 1364.e1-14. doi: 10.1016/j.jaci.2013.11.030. Epub 2014 Jan 22. http://www.ncbi.nlm.nih.gov/pubmed/24461581 |
| Yip et al. 2015 | Kwok-Ho Yip, PhD, Natasha Kolesnikoff, PhD, Chunping Yu, BSc, Nicholas Hauschild, BSc, Houng Taing, BSc, Lisa Biggs, BSc, David Goltzman, MD, Philip A. Gregory, PhD, Paul H. Anderson, PhD Michael S. Samuel, PhD, Stephen J. Galli, MD, Angel F. Lopez, PhD and Michele A. Grimbaldeston, PhD: "Vitamin D3 represses IgE-dependent mast cell activation via mast cell-CYP27B1 and -vitamin D receptor activity" J Allergy Clin Immunol. Author manuscript; available in PMC 2015 May 1. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4154631/ |
| Yu et al. 2014 | Yu Y, Blokhuis BR, Garssen J, Redegeld FA: "Non-IgE mediated mast cell activation." Eur J Pharmacol. 2015 Jul 8. pii: S0014-2999(15)30144-8. doi: 10.1016/j.ejphar.2015.07.017. https://pubmed.ncbi.nlm.nih.gov/26164792 "There is a plethora of stimuli, such as IgG, complement components, TLR ligands, neuropeptides, cytokines, chemokines and other inflammatory products, that can directly trigger mast cell degranulation, cause selective release of mediators, and stimulate proliferation, differentiation and/or migration. Moreover, some of these stimuli have a synergic effect on the IgE-mediated mast cell activation. [...] In this review, we discuss current knowledge on non-IgE stimuli for (human) mast cells." |
![[Logo MCAD]](../pics/logo_mcas_160x160_bkg045552.png)